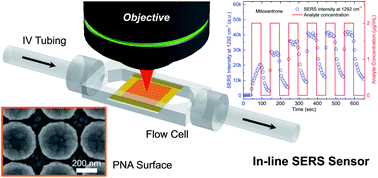
chemistryworld: “Recent research, led by Brian Cunningham at the University of Illinois in the US, has produced biomedical tubing that uses surface enhanced Raman spectroscopy (SERS) to monitor the contents and concentrations of drugs within a patient’s IV line. The plasmonic nanodome array surface enhances the Raman signals. The tubing could detect 10 pharmaceutical compounds with reproducible signals for a period of up to five days. For four of the drugs, the signal magnitude was dependent upon the drug concentration and combinations of compounds could also be detected, giving a much more detailed picture of a patient’s medication.†– This is great work being done by the University of Illinois. I’ve contemplated something like this in the past.
Category: Medication Safety
-
Accuracy of preparation of i.v. medication syringes for anesthesiology [article]
Here’s an interesting article from the January issue of AJHP that talks about the accuracy of medication syringes used in surgical procedures. Some of the findings are a bit unnerving: “18% of preparations deviated from the declared dose by ±20%, 8% deviated by ±50%, and 4% deviated by ±100%“. Humans, we’re just not all that good at things like this.
Accuracy of preparation of i.v. medication syringes for anesthesiology
Cyril Stucki, Anna-Maria Sautter, Adriana Wolff, Sandrine Fleury-Souverain and Pascal BonnabryAbstract
Purpose: The results of a study of the accuracy of i.v. medication preparation by anesthesiologists are presented.
Methods: The accuracy of syringe preparation was assessed by analyzing the contents of 500 unused syringes collected after adult and pediatric surgery procedures. The collected syringes contained various i.v. medication formulations representative of different preparation techniques: atracurium 1, 2.5, and 5 μg/mL and fentanyl 10, 20, 25, and 50 μg/mL, which required serial dilution after withdrawal of the drugs from ampuls; thiopental 5, 25, and 50 mg/mL, prepared by diluting reconstituted powdered drug from vials; and lidocaine 10-mg/mL solution, which was withdrawn directly from the ampul into a syringe. Variances between actual and labeled drug concentrations were determined via a validated ultraviolet–visible light spectro-photometry method.
Results: Overall, 29% of the evaluated syringes were found to contain drug concentrations outside the designated range of acceptability (±10% of the targeted concentration); 18% of preparations deviated from the declared dose by ±20%, 8% deviated by ±50%, and 4% deviated by ±100%. In one instance, the actual drug concentration was at variance with the labeled concentration by >100%. In 4% of cases ( n = 20), discrepancies exceeded 100%, suggesting not just imprecision but errors in the preparation process, such as incorrect dilution calculations and selection of the wrong medication vial by the syringe preparer.
Conclusion: Analysis of different i.v. formulations of four medications prepared in syringes by anesthesiologists revealed a high rate of discrepancies between ordered and actual drug concentrations, suggesting a need for increased institutional efforts to prevent errors during the preparation process.
Am J Health-Syst Pharm. 2013; 70:137–42
-
Excessive acetaminophen dosing in hospitals more common than you might think
 Archives of Internal Medicine: “A total of 14 411 patients (60.7%) were exposed to acetaminophen, of whom 955 (6.6%) exceeded the 4 g per day maximum recommended dose. In addition, 22.3% of patients who were 65 years or older and 17.6% of patients with chronic liver diseases exceeded the recommended limit of 3 g per day.†Arch Intern Med. Published online November 12, 2012
Archives of Internal Medicine: “A total of 14 411 patients (60.7%) were exposed to acetaminophen, of whom 955 (6.6%) exceeded the 4 g per day maximum recommended dose. In addition, 22.3% of patients who were 65 years or older and 17.6% of patients with chronic liver diseases exceeded the recommended limit of 3 g per day.†Arch Intern Med. Published online November 12, 2012Not surprising at all. Any pharmacist that’s worked in a hospital setting can tell you that an average patient profile is riddled with potential excess acetaminophen dosing. We used to have order sets for post-op patients that contained acetaminophen 650mg Q 4 hrs prn pain/temp plus Darvocet N-100 2 tablets Q 4 hrs prn pain plus Vicodin 1-2 Q 4 hrs prn pain thrown in for good measure. When pharmacy would object to these order sets the hospital would simply say that no one would ever give all of those to one patient. It’s common sense after all. You’d be surprised what people will do.
Medscape has expanded information on the article if you don’t have credentials to read the full Archives article.
-
Combination lock to prevent blood transfusion errors? Why not
medGadget: “Typenex Medical, a Chicago, Illinois company, has created a solution that pretty much eliminates the possibility for errors. The system utilizes a combination lock on the blood bag that will only open using a code printed on the patient’s armband. If a clinician accidentally attempts to open the bag using another patient’s code, it will stay closed and the transfusion will not happen.†– Simple, yet effective. Interesting concept, no?
The product is called FinalCheck.
-
More on the meningitis outbreak caused by contaminated steroid injection
Things just keep getting worse: death toll rose to 14 and people affected was up to 172 in 11 states as of this afternoon. It’s difficult to find accurate information on the exact cause of the meningitis, but it appears that most of the cases are related to either Aspergillus or Exserohilum.
Fungal infections are notoriously difficult to treat, especially when they’re in the central nervous system (CNS). The CNS is designed like a fortress to keep things out, like fungus and bacteria, thus keeping you safe and healthy. Unfortunately it doesn’t discriminate and does a great job of keeping medications out as well. That’s why it’s hard to treat infections in the CNS.
I’ve been involved with several meningitis cases over the years, but rarely those involving a fungus. The outcome generally depends on several variables including how quickly the infection is discovered, how soon treatment is started, how aggressive the treatment is – you can never be too aggressive when treating meningitis – and the general health of the person you’re treating. A little divine intervention is always desirable as well. However, as I mentioned above, meningitis is difficult to treat and the outcomes associated with fungal meningitis aren’t great.
The CDC has released treatment recommendations. You can find them at the ASHP Pharmacy News site here.
“The Centers for Disease Control and Prevention (CDC) recommends i.v. voriconazole and liposomal amphotericin B as initial therapy for patients who meet the current case definition for fungal meningitis.
According to CDC, the antifungal therapy for patients with meningitis should be administered in addition to routine empirical treatment for potential bacterial pathogens.
CDC Medical Epidemiologist Tom Chiller said during an October 10 conference call that broad-spectrum antifungal therapy is advisable because it is “unclear as to how many potential fungal pathogens could be involved” in the outbreak.
For patients who meet CDC’s current case definition for fungal meningitis, the recommended dosage of voriconazole is 6 mg/kg administered every 12 hours. Chiller said the dosage should be maintained “for as long as the patients tolerate it.”
Liposomal amphotericin B should be administered intravenously at a dosage of 7.5 mg/kg/day, according to CDC. The agency stated that liposomal amphotericin B is preferred over other lipid formulations of the drug.
The optimal duration of therapy is unknown but is presumed to be lengthy.â€
Emphasis above is mine.
-
Outsourcing sterile product preparation and the importance of quality assurance
I’m sure you’ve heard about the recent meningitis outbreak tied to a contaminated batch of preservative-free methylprednisolone acetate. The story has received significant attention as more that 100 people have been sickened and as many as eight have died as a result of receiving an injection of the contaminated steroid (this data is already out of date since I started composing this post yesterday).
(more…) -
A trip to IHOP and more thoughts on color
A trip to the local IHOP (@IHOP) this morning for breakfast with my family reminded me of something I saw a couple a weeks ago and this post about the use of color in pharmacy labels. It’s a big of a stretch, I know, but the things that pop into one’s mind aren’t necessarily controlled by logic.
(more…) -
Forcing re-entry of patient ID cuts wrong-patient errors
You know how websites make you double enter your email address and password when you sign up for a service? Well, apparently that’s not a bad system for making sure you have the right patient during order entry. You’d think we would have figured that out a while back, but then again this is healthcare we’re talking about; equation for healthcare technology “innovation” is ([today’s technology] -10 years).
The study found that requiring clinicians to re-enter patient IDs resulted in a 41% reduction in wrong-patient orders. Single-click confirmation of patient ID reduced wrong-patient orders by 16%. It’s not all peaches and cream though. The study found that double entry increased order entry by 6.6 seconds. Oh no!
Understanding and preventing wrong-patient electronic orders: a randomized controlled trial (J Am Med Inform Assoc. 2012 Jun 29Â )
Abstract
Objective:Â To evaluate systems for estimating and preventing wrong-patient electronic orders in computerized physician order entry systems with a two-phase study. Materials and methodsIn phase 1, from May to August 2010, the effectiveness of a ‘retract-and-reorder’ measurement tool was assessed that identified orders placed on a patient, promptly retracted, and then reordered by the same provider on a different patient as a marker for wrong-patient electronic orders. This tool was then used to estimate the frequency of wrong-patient electronic orders in four hospitals in 2009. In phase 2, from December 2010 to June 2011, a three-armed randomized controlled trial was conducted to evaluate the efficacy of two distinct interventions aimed at preventing these errors by reverifying patient identification: an ‘ID-verify alert’, and an ‘ID-reentry function’.
Results: The retract-and-reorder measurement tool effectively identified 170 of 223 events as wrong-patient electronic orders, resulting in a positive predictive value of 76.2% (95% CI 70.6% to 81.9%). Using this tool it was estimated that 5246 electronic orders were placed on wrong patients in 2009. In phase 2, 901 776 ordering sessions among 4028 providers were examined. Compared with control, the ID-verify alert reduced the odds of a retract-and-reorder event (OR 0.84, 95% CI 0.72 to 0.98), but the ID-reentry function reduced the odds by a larger magnitude (OR 0.60, 95% CI 0.50 to 0.71).
Discussion and conclusion:Â Wrong-patient electronic orders occur frequently with computerized provider order entry systems, and electronic interventions can reduce the risk of these errors occurring. -
Prenteral nutrition error [from #ISMP]
From the latest ISMP Medication Safety Alert!, a mix up between an adult parenteral nutrition (PN) template in an electronic health record (#EHR) and one for pediatrics.
The big difference between these two is how you order electrolytes; it’s a really big difference.
The most shocking part of all this was that the error made it’s way through the physician that ordered it, a pharmacist that “entered the PN order” (I’m assuming in the compounding application), the “trained technician” that prepared it – missing the fact that the bag contained a whooping 2600mL of sterile water, the pharmacist that checked it, and finally the nurse that hung it. Swiss cheese anyone?
(more…) -
Warning labels on outpatient prescription vials not so great after all
 Everyone has seen them, I know you have. Those little colored labels that the pharmacy slaps on your bottle when you get a prescription: “May cause drowsinessâ€, “Avoid excess sunâ€, “Do not take aspirin products without doctor approval†and so on. There are a ton of them. I remember seeing them lined up in front of me when I was working retail. Sometimes it became a game to see how many you could fit on the bottle without covering up valuable information for the patient. I’ve also been in pharmacies where the warning labels were simply printed alongside the medication label.
Everyone has seen them, I know you have. Those little colored labels that the pharmacy slaps on your bottle when you get a prescription: “May cause drowsinessâ€, “Avoid excess sunâ€, “Do not take aspirin products without doctor approval†and so on. There are a ton of them. I remember seeing them lined up in front of me when I was working retail. Sometimes it became a game to see how many you could fit on the bottle without covering up valuable information for the patient. I’ve also been in pharmacies where the warning labels were simply printed alongside the medication label.Well, it appears that this tradition may not be the best way to warn patients about potential issues with their medication. I mean, who really reads those things anyway?
A small study recently published in the journal PLoS ONE took a look at these warning labels and determined that people really don’t pay attention. Not surprising.
(more…)